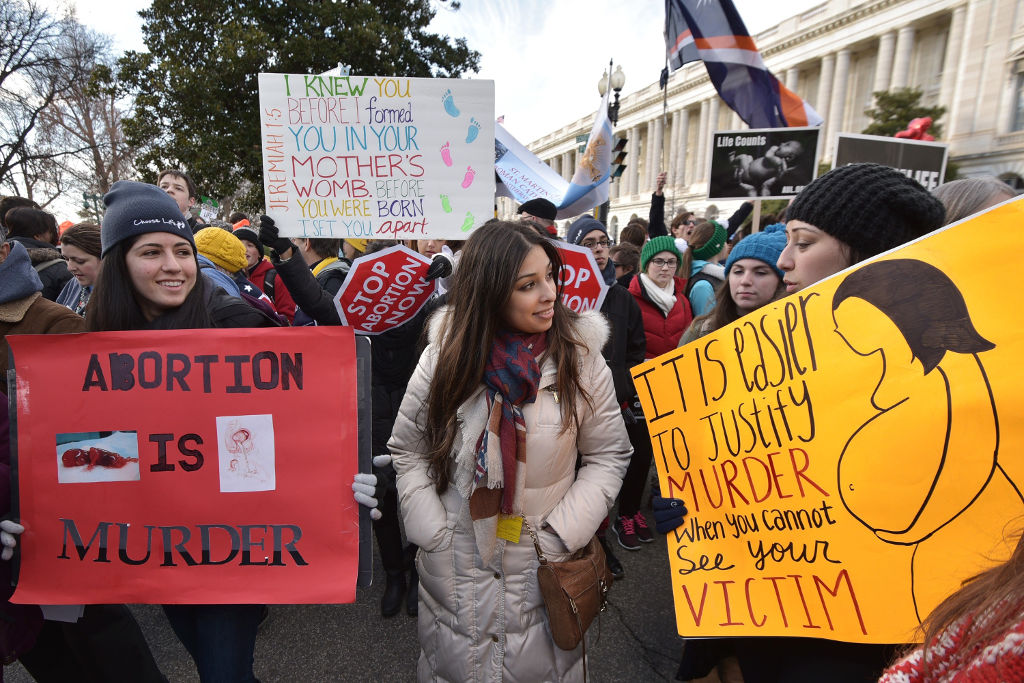The Barriers To Access A Medical Abortion In Australia Are Shocking And Unfair
It should not be this hard (or expensive).

Australia is a bit of a strange and backward place when it comes to abortion laws. Not only do the rules and restrictions vary wildly state-by-state, the cost to access an abortion is not regulated, and can therefore be prohibitively expensive.
It’s 2017 and Labor MP Tanya Plibersek is again addressing a large group of people about the prohibitive cost of a medical abortion. In a speech to Emily’s List last month, Plibersek pointed out that “for many women abortions are unaffordable and unattainable”. And she’s right. Despite the fact that the medical abortion drug is on the Pharmaceutical Benefits Scheme (PBS) and generally costs as much to purchase as most antibiotics, women are still paying upwards of $500, sometimes closer to $1,000 for the entire medical abortion process (which can include doctor’s consultations, ultrasounds, counselling, aftercare and the now inexpensive drug itself).
The issue here is access; across the country, women are paying wildly different prices to access the same services. Medical abortion services are provided by some GPs, a handful of small private clinics, the tele-abortion provider Tabbot Foundation, and also the non-profit organisation Marie Stopes International (AU). Because of their large network of metropolitan and regional clinics, Marie Stopes is likely the chief provider of medical abortions in Australia — and their prices are also the most expensive.
This confusing, unregulated and prohibitive price discrepancy among providers combines with the complicated Australian abortion laws to create an environment where, for many women, access to a safe abortion is virtually impossible.
The procedure, which Plibersek has said is one of the most common medical procedures Australian women will experience in their lives, is being held back from a public who, in most Australian states and territories, has every legal right to access it (and the universal healthcare that should make the procedure mercifully affordable). But that’s not happening, and that is shocking and critically unfair.
Australia’s Complicated Relationship With Abortion
It might surprise you to know that abortions are not legally accessible in every part of Australia. If you live in Victoria, the ACT, Tasmania, Western Australia or the Northern Territory, abortion is legal and accessible up to various different time periods (with many different regulations). In Victoria, for example, abortion is legal up to 24 weeks, and accessible beyond with approval from two doctors. In Western Australia abortion is legal up to 20 weeks and highly restricted beyond, as well as being restricted for individuals under 16 years old.
But in NSW and Queensland, abortion is yet to be officially decriminalised in the State Crimes Acts, and in South Australia the procedure still faces some restrictions. Women who have chosen to terminate a pregnancy in these states are often forced to travel across state lines to access the procedure — and many have resorted to riskier and more impractical options to get the healthcare they need.
For women who do make it to an abortion provider, in many states they lack the protection of exclusion zones, and so already vulnerable women are sometimes harassed and intimidated by “pro-life” protestors as they access the delicate procedure.

Source: Flickr/David Jackmanson
Then there’s the cost: a surgical abortion, which needs to be performed with a nurse and an anaesthesiologist in a day surgery, can understandably cost upwards of $600. This is why the medical abortion was introduced in Australia: a safe, non-surgical option for women who are eight weeks pregnant or less, which can be completed at home over 24-48 hours.
One of the most widely-used abortion providers in Australia, Marie Stopes, says on its website that a medical abortion can cost “from $440”, but reports from customers reveal the organisation often charges much more — up to $800 or over for the procedure, and prices are highest in rural and remote areas, like far-north Queensland.
This huge price difference — depending on the services women access — for a medical abortion seems unnecessary and distinctly unfair. Plibersek has pointed out “women seeking abortions are charged more for medical terminations than they are for traditional surgical terminations”. So why does the supposedly cost-effective procedure still cost so much?
Let’s Talk Dollars
The abortion drug, which has been imported to Australia by Marie Stopes’ pharmaceutical arm since 2012, was once exorbitantly expensive. Jacquie O’Brien, the head of Public Affairs at Marie Stopes Australia, told Junkee, “In 2012 we thought — being an organisation that is dedicated to access — it aligns with our mission if we bring this drug into the country. And at the time it cost millions of dollars, which is a big investment for any organisation but particularly for a not-for-profit. So we did that because it was important that we brought the drug into the country.”
As Health Minister in the Rudd and Gillard governments, Tanya Plibersek fought tirelessly to advance the legislation necessary to include the abortion drug on the PBS. And in June 2013, Julia Gillard’s last act as prime minister was to sign off on this legislation. The cost of the actual medical abortion drug (excluding doctor’s consultation) dropped from upwards of $800 to as little as $12 for concession card holders, or around $38 for those on Medicare.

The change to the price of the drug was accompanied by a new scheme allowing GPs to train up so they could prescribe the drug from their practice, making a medical termination generally more accessible for low-income Australians and people in rural or remote areas. This training scheme is run by Marie Stopes — part of their responsibility as the medical abortion drug’s sponsor in Australia. Additionally, an over-the-phone service was introduced to assist in dispensing the procedure to remote Australians.
But this measure has done shockingly little to decrease the price of a medical abortion at some providers. Despite the fixed cost of the drug itself, the accompanying consultation fees can vary wildly.
The medical abortion — which involves visiting a consulting GP or a clinic to get all the necessary tests and ultrasounds, to receive counselling support and to obtain a script to purchase the pill at a pharmacy — is a process that is largely self-directed by the woman accessing it. Once a GP or clinician has signed off on your abortion and you’ve received the medical abortion drugs, you are able to complete the abortion at home. Generally you are required to follow up with your provider to ensure the procedure was successful, but the process is minimally invasive (there is no surgery involved) and can be performed comfortably at home.
Considering this: how can there be such a vast difference in price across providers? Junkee did some investigation.
Dr Catherine Insley, one of few Sydney GP abortion providers, who practices at East Sydney Doctors, quoted the cost for a medical abortion from her practice (excluding the drug cost) at $250. She also noted that, with a Medicare rebate, the out-of-pocket cost would be closer to $120. Other GPs who dispense the service (in Victoria) quoted Junkee between $250-$350 for a consultation, excluding the minimal cost of purchasing the pill.
Many small-clinic, public and private abortion providers like The Women’s Clinic or the Monash Family Planning Service in Melbourne, have quoted similar prices, where others refuse to designate a flat fee. The Better Health Channel (a Victorian government health initiative) has provided a reasonably comprehensive list of providers and prices for that state’s services.
Additionally, the cost of a tele-abortion at the Tabbot Foundation — where women without access to a supportive healthcare provider can have their consultation over the phone — is quoted at $250 for those with Medicare. (Marie Stopes also offers a tele-consultation service, advertised at upwards of $290 excluding the cost of medication).
If you head to a private clinic, the rate increases. Marie Stopes quotes a base cost of $440 for its medical abortion. They are also one of few providers who only quotes a base cost online (suggesting the price can increase) and rolls the cost of unlikely complications into their pricing scheme. Marie Stopes is far more widely accessible across the country than other providers who offer more cost-effective procedures.
So, even though many in Australia are trying desperately to make abortion accessible, the procedure is still inaccessible for far too many Australian women.
Bad Blood Between Providers
It’s not quite clear with whom the blame for this clusterfuck lies. Many of the GPs Junkee has spoken to are blaming Marie Stopes for monopolising the process and overpricing their procedures to cover other costs in their organisation; while Marie Stopes suggests the GPs are not advertising the true, all-inclusive cost of a medical abortion.
Still, legions of practitioners in the industry agree on one thing: there are still many roadblocks to accessing a medical abortion that need to be removed to assist the swathe of Australian women who are currently not able to access the procedure that is their legal right.
“It’s just knowing where to go and how much they cost,” Dr Insley explains when I ask her who in Australia has access to the medical abortion. “Theoretically it’s any woman, really. But I think a lot of women are scared off because they think it might not work properly.”
The complex political deadlock around abortion law can mean that many women are given the wrong information about how these procedures work, but Dr Insley assured Junkee that “on the whole, most women tolerate it well.
“They’re more in control in the medical termination. I find there’s less of a psychological effect with medical termination, because [women are] more in control and they’re sort of doing it themselves rather than being asleep and somebody else doing it.”
For the small percentage of women who undertake the procedure and encounter issues, the 24-hour aftercare line is actually run by Marie Stopes, so regardless of where you undertake the procedure, at some point in the process Marie Stopes will be involved in your medical abortion.
This small percentage of women who experience what the industry refers to as “retained product” (when some of the pregnancy materials remain in the uterus after the abortion procedure is completed), is part of why the price is inflated at Marie Stopes. O’Brien tells Junkee that the (slim) risk of having to return for surgery to remove retained product is built into the price — and while Marie Stopes estimates the risk of experiencing these difficulties sits between one and five per cent, Dr Insley asserts it’s more like one or two percent.
“I think [Australian women have] been overcharged by the clinics.”
Many practitioners, Dr Insley included, have a problem with how involved Marie Stopes is in dispensing medical abortions across the country. “They’ve got a monopoly on it, really,” Dr Insley explains. “They’ve come to some agreement with the TGA [Therapeutic Goods Administration] and the government that if they’re the only provider then the price is set, but then nobody else is allowed to compete with them.”
Where some practitioners see an issue, Marie Stopes argues that their prices support “the cost of running clinics across states and territories”. O’Brien tells Junkee, “regional access is really difficult, because it’s very expensive to run a clinic in a region” which can account for some of the additional costs associated with accessing the procedure at Marie Stopes. “It can be really quite expensive,” she says. “We find that in Northern Queensland especially.”
Dr Insley is a little more cynical about what your abortion costs cover in a Marie Stopes clinic. “A lot of the clinics, especially Marie Stopes, well all of them really, they spent a huge amount on marketing,” says Dr Insley, “They are completely dependent on coming up at the top of the list of Google, and most women just phone the first number, you know?”
It certainly appears as though there’s some bad blood between Marie Stopes and the smaller providers, if only because Marie Stopes drives up the price of the procedure for those practitioners who do not have the protection of a nationally recognised brand. “I think [Australian women have] been overcharged by the clinics, because there’s not many people who provide this,” Dr Insley reasons. “I mean it’s availability, isn’t it?
“I think Marie Stopes are making, you know… they make a lot of money,” Insley goes on. “A lot of GPs believe that Marie Stopes is a good place to refer people to because then they pump money back into the third world for reproductive service and things, but they actually don’t. None of the money from Australia goes overseas. It stays within Australia and builds the business here in Australia.”
And while Marie Stopes hasn’t denied these charges — in fact the company’s chief operating officer in Australia, Jamal Hakim, has told BuzzFeed Australia, “We are a not-for-profit and we are mission-driven, but we’re not about losses either” — O’Brien is a little rankled when I test Dr Insley’s assertions on her.
“It’s actually a lot more complicated,” she says. When I ask her what can be done to even out the price disparity, she replies, “I think what is really important is if providers are really clear about: for this price this is the service that you get, this is what it covers, and this is what it doesn’t cover.
“As providers we have a responsibility to be educating patients when they come to us, because a lot of them won’t know. You know, many women will only come to us once or twice, it’s not a procedure that women have often. But still there’s a lot of women who are accessing it. So that’s probably the key suggestion: being upfront about what is involved in the cost, and what’s not.”
So, What Can Be Done?
It seems clear that these kinds of problems arise when medical services do not receive adequate support from the government. If the government supported abortion services as much as they did other common medical procedures, perhaps clinics would not have to set sky-high prices. If the government opened up the importation and dispensing of the medical abortion drug, perhaps one organisation would not have this so-called “monopoly” on all elements of the procedure, or would not have so many operational costs to cover.
And if more women were educated about what the procedure is, what’s involved and how much it should cost, perhaps less Australian women would be in the position of having to go shopping for an affordable abortion, or to engage in “abortion tourism” (travelling interstate for the procedure), as many currently do. Clinics and GPs providing abortion services should be supporting each other, not harbouring resentment over their noble contributions to an already broken system.
As Tanya Plibersek said in her Emily’s List speech: “Our outdated laws are a serious barrier to the provision of health care. Women seeking abortions are charged more for medical terminations than they are for traditional surgical terminations. In a survey earlier this year, one in three women said they found it difficult to pay for their abortion. Two thirds needed financial assistance and had to miss paying bills or cut back on food to afford it.”
It’s time for our governments to come together in aid of women, to disentangle abortion services from politics and morality and complications, and to finally regulate a service that is at best poorly organised, at worst actively deterring Australian women from seeking help to control their reproductive futures.
—
Matilda Dixon-Smith is Junkee’s Staff Writer. She tweets at @mdixonsmith.